Prokar Dasgupta, professor of surgery at King’s College, London, and chair of the Centre for Robotics at The London Clinic, explains how robotic surgery has become democratised.
Twenty years ago, The London Clinic became the first independent hospital in the UK to launch a robotic surgery programme, initially using the original da Vinci system from Intuitive Surgical, California, for urological conditions like prostate cancer.
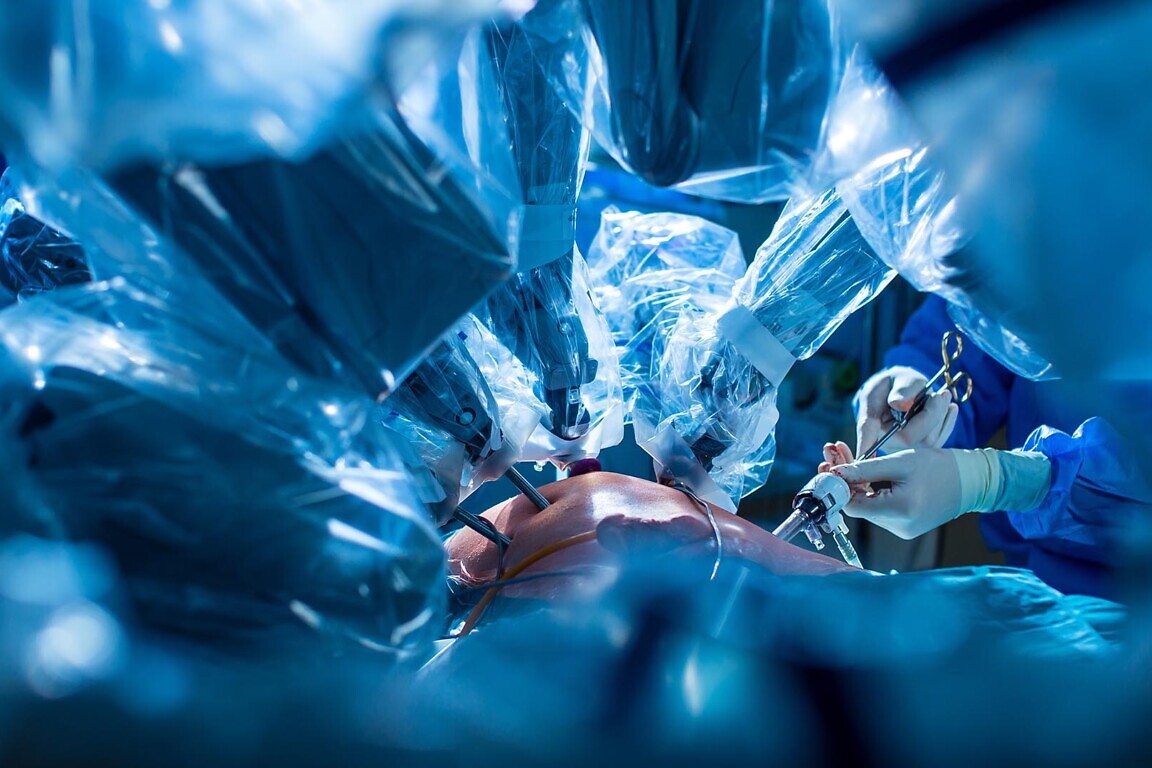
Since then, we have adopted every version of this robot as it has evolved. The 3D-HD magnified vision and fine robotic wrists capable of operating without tremor (even if the surgeon has one) have transformed keyhole surgery forever.
Using this technology, patients experience less blood loss, reduced pain, shorter hospital stays and faster recovery. Despite initial concerns over cost, studies have since demonstrated that the minimally invasive technology is cost-effective for most cancers when compared to open surgery. As a result, other specialties, including gynaecology, lung, bowel and throat surgery have also embraced this technology for the benefit of their patients. Our robotics programme has continued to expand, incorporating robots for orthopaedics, spinal surgery and benign enlargement of the prostate.
Renewed interest in automation
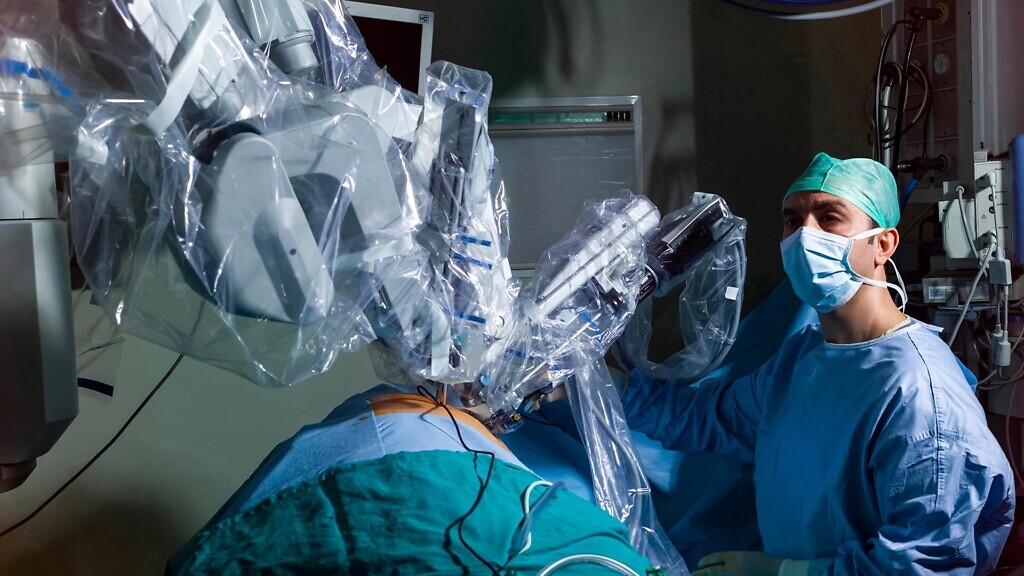
Today, the remarkable da Vinci robot faces stiff competition from other international manufacturers, with about 50 new companies entering the market. To challenge the current gold standard, these systems must match or surpass da Vinci’s capabilities.
The alternative is that they market themselves as significantly cheaper options, thus attracting a wider variety of institutions who could not afford the da Vinci. Common features in these new systems include open consoles, enhanced 3D vision, lighter instruments and greater portability.
There is also renewed interest in automation, the origin of which can be traced back to John Wickham, the world’s first robotic surgeon. One example is the Smart Tissue Autonomous Robot (STAR) which can suture bowel tissue more effectively than a human hand in animal models.
Another example, a water-jet robot from Procept Biorobotics, takes inspiration from Wickham’s original robot: the PROBOT, and creates a channel inside an enlarged prostate, much like coring an apple, to improve urine flow. The London Clinic now performs the highest volume of this procedure in the UK.
New robots entering the market hold the potential to reduce the cost of robotic surgery to levels comparable to traditional laparoscopy (keyhole surgery without robots), although the initial hardware investment may still be substantial.
Cambridge Medical Robotics, with its UK-designed Versius robot, and Medtronic, with its HUGO robot, have introduced competitive cost-per-procedure models as part of a comprehensive package.
Another example is the Mantra system from India, which has received strong support from the government of India due to its significantly lower cost. The entry of such systems into the market has made robotic surgery more appealing to hospitals with high volumes of open and laparoscopic surgeons, looking for multidisciplinary expansion.
Two other exciting developments in the world of robotics are artificial intelligence (AI) and telesurgery. AI isn’t a new concept, with origins dating back to the genius of Alan Turing, whose ground-breaking decoding skills played a pivotal role in shaping the outcome of World War II.
Its current applications are transforming healthcare. Machine learning, a subset of AI, uses decision-making computer algorithms to process specific data. For example, a prostate recognition algorithm could teach a machine to distinguish between prostate cancer and healthy tissue, thus reducing the variability in MRI readings by radiologists.
AI can also analyse video recordings of surgeons performing robotic surgery and convert them into automated performance metrics that highlight which surgical gestures yield the best patient outcomes.
With large language models revolutionising AI, we can now create personalised digital twins and 3D models to enhance the precision of robotic surgery – an advancement that was unimaginable just two decades ago.
Telesurgery compatible
The UK government, amongst others, has invested billions in AI to attract new talent and maintain its position as a global leader in this rapidly evolving field. National programmes such as the Trustworthy Autonomous Systems and the international ecosystem Responsible AI UK, promote collaboration between countries, companies and civil society for the benefit of the patient.
I had the distinct privilege of attending the AI Fringe in 2023 during the inaugural AI Summit in the UK, and again in 2025 to align with the AI Summit in Paris. During these important events it became clear that the focus of AI has moved onto socio-technical solutions rather than just technical, which helps to reduce the risk of AI technology becoming an existential threat to humanity.
Robotic surgery has been further democratised by low-latency 5G and high-speed fibre connectivity. The Internet of Skills has made remote robotic telesurgery and mentorship easily accessible, regardless of the expert surgeon’s location.
Several Chinese companies have developed robots that are telesurgery compatible, sparking renewed interest in remote surgery, a field first pioneered over 20 years ago.
The potential impact of these developments on patient care will undoubtedly be of considerable interest to the broader surgical community.